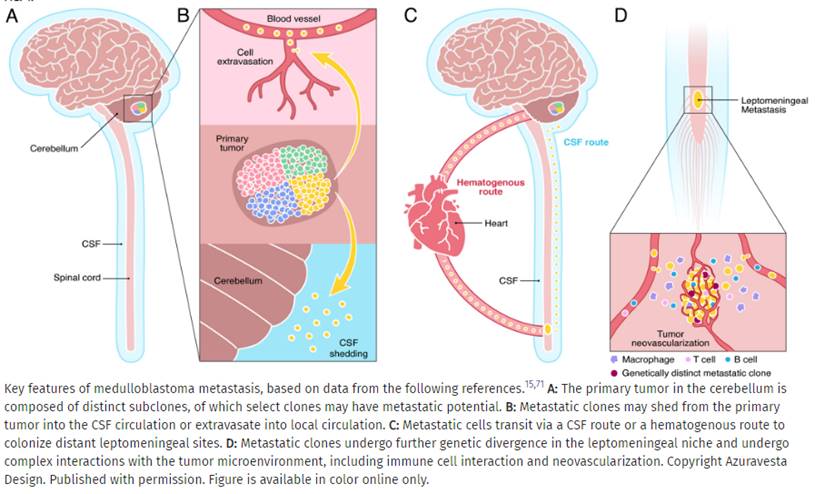
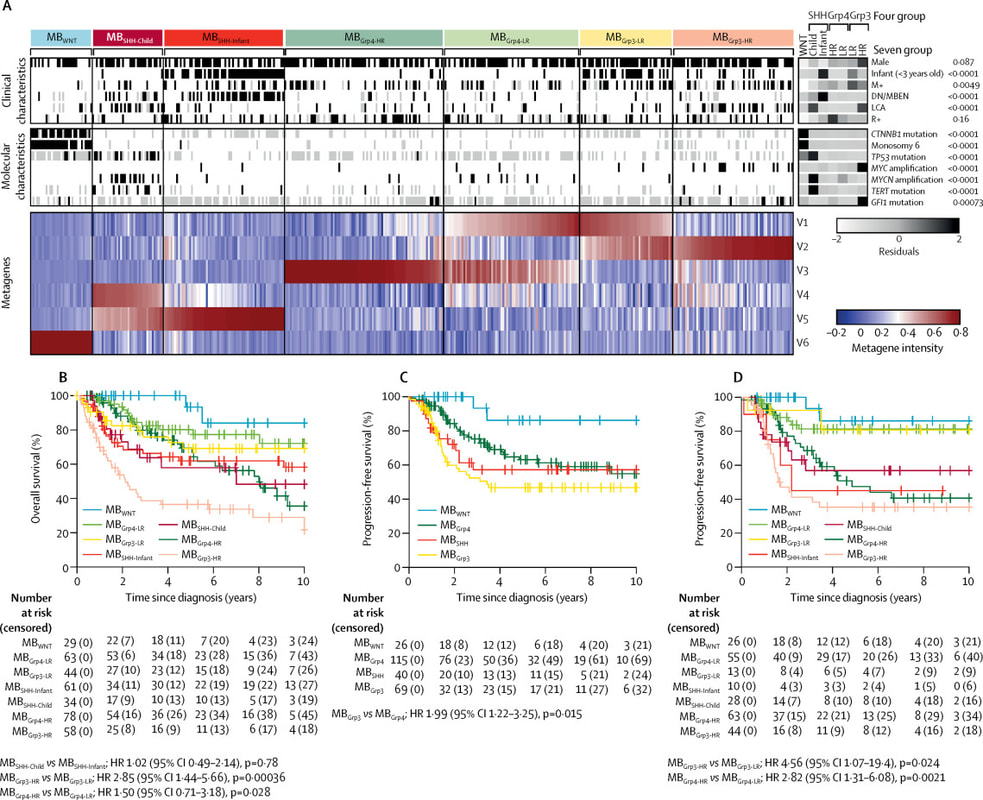
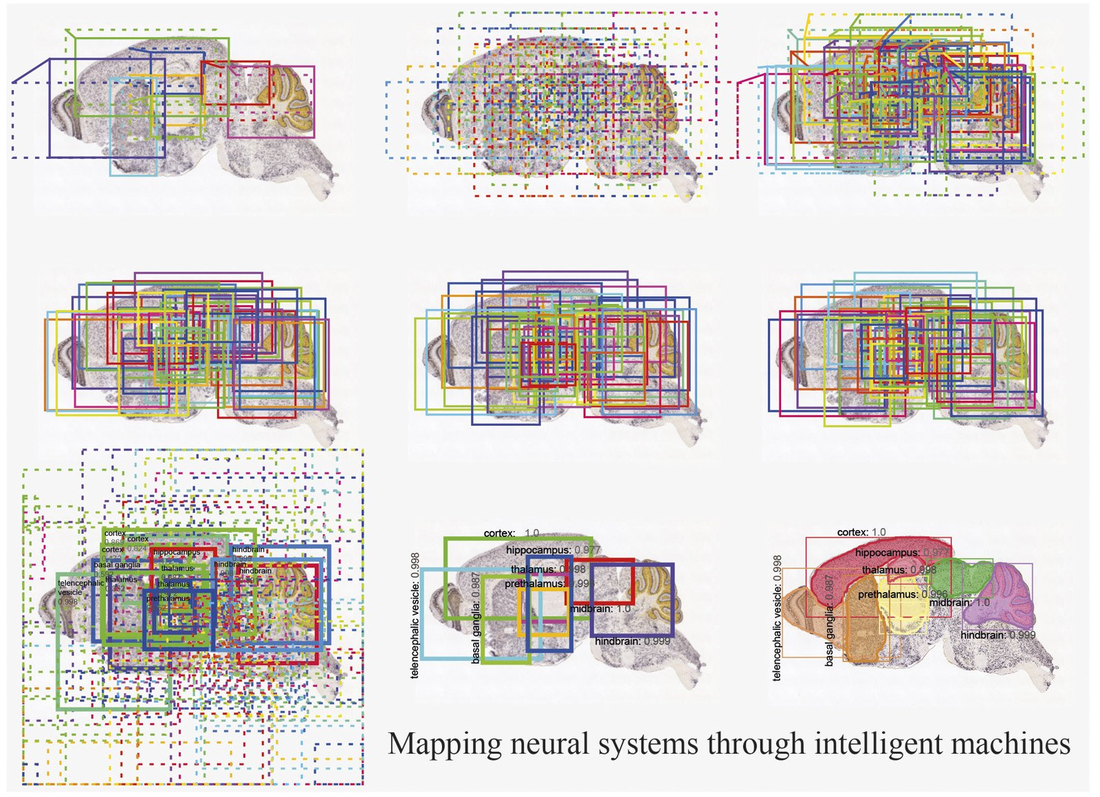
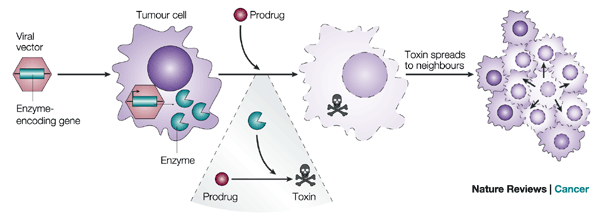
Blog Author: Archita KhaireMedulloblastoma is the most prevalent brain tumor type in children. It is also called a cerebellar primitive neuroectodermal tumor (PNET)—that starts in the region of the brain at the base of the skull, called the posterior fossa. In the United States, about 400 children are diagnosed with #medulloblastoma every year. The survival rate of Medulloblastoma is about 70%. Image Credit: JNS Journal of Neurosurgery Common symptoms of Medulloblastoma include Headaches, Nausea, Vomiting, Clumsiness or similar balance problems, and vision problems. Sometimes Medulloblastoma enters into the ventricles of the brain causing a buildup of cerebrospinal fluid which can result in symptoms of an enlarged head. Based on gene changes in the cancer cells they are grouped into 4 subtypes: WNT, SHH, Group III, Group IV. SHH (also know as Sonic HedgeHog) is the most common in adults. Diagnosis MRI and CT scan and common methods to diagnose the Medulloblastoma. Machine learning algorithms have enabled neurosurgeons to detect gene mutations associated with cancer within the plasma. However, this type of early diagnosis does not work in pediatric brain cancers because these cancers often have very few mutations. Instead, certain critical genes are turned on or turned off by epigenetic changes that regulate their activity in cases of pediatric brain tumors. There is evidence that DNA methylation changes at cytosine-phosphate-guanine (CpG) sites are associated with cancer. Researchers are performing Quantitative epigenetics to detect biomarkers of Medulloblastoma. Image Credit: The Lancet Oncology, https://doi.org/10.1016/S1470-2045(17)30243-7 Treatment Surgery is the most common treatment to remove the medulloblastoma tumor cells. Doctors are using enhanced imaging techniques (Cortical mapping using artificial intelligence) that enables the identification of areas of the brain that control the senses, language, and motor skills. Image Credit: https://sciglow.com/developing-brain-maps-through-artificial-intelligence/ Researchers at John Hopkins are working on the possibility of using biodegradable, lab-engineered nanoparticles that could kill medulloblastoma tumor cells. The #nanoparticles are diffused within the tumor due to the increased permeability of the tumor vessels, however; the low clearance prohibits the formulations from getting out. This methodology is mostly used for siRNA but not for DNA plasmid delivery. It is a therapeutic strategy commonly known as Suicide Gene Therapy. Artificial intelligence is opening a new era of nano medicine to treat cancers. To improve the efficacy of gene therapy, researchers are developing machine learning models that could predict the shapes and sizes of nanoparticle delivery systems, a form of drug delivery to cancer site, the most effective path of delivery.
Future Scope Researchers are working to learn more about medulloblastoma, ways to diagnose it in early stages, non-invasive ways to treat it and prevent from reoccurrence. Proton therapy is one of the area where use of artificial intelligence is being experimented to improve accuracy and efficacy of the treatment. References
Comments are closed.
|
Page HitsAuthorArchita Archives
January 2023
Categories |

 RSS Feed
RSS Feed