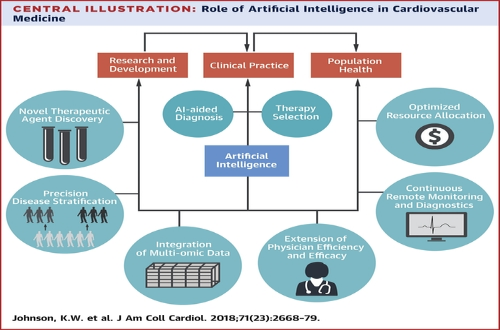
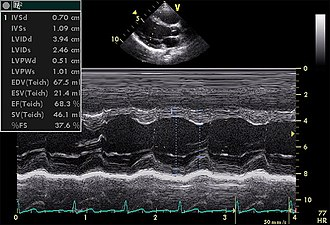
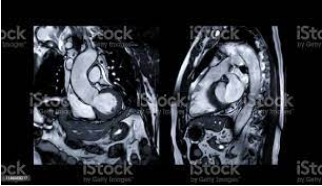
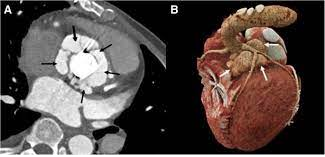
Blog Author: Kulani MelakuCardiovascular diseases(CVDs) affect the heart and blood vessels of the body. This disease is the number one cause of death worldwide. There are many types of CVDs, i.e., Arrhythmia, Valve Disease, Coronary Artery Disease, Heart Failure, Peripheral Artery Disease, Aortic Disease, Congenital Heart Disease, Pericardial Disease, Cerebrovascular Disease, and Deep vein thrombosis are the common ones. AI can help cardiac care in 3 major areas. AI Aided Diagnostic Machine learning, deep learning, and cognitive computing are examples of AI approaches that have the potential to transform how cardiology and cardiovascular care are conducted (for example, how we generate knowledge, evaluate data, and make decisions), particularly in cardiovascular imaging. A. Echocardiography Echocardiogram in the parasternal long-axis view, showing a measurement of the heart's left ventricle #Echocardiography is a test that uses sound waves to produce live images of your heart. The image is called an echocardiogram. This test allows your doctor to monitor how your heart and its valves are functioning. AI tools, in particular machine learning, provide new possibilities to enhance the accuracy of image interpretation in clinical echocardiography practice, especially between non-expert clinicians. The algorithm integrated into the software is capable of automatically calculating the following in a few seconds: the volumes of the left chambers, the systolic flow, and the ejection fraction of the LV from the data acquired with 3D echocardiographic techniques. Researcher Sengupta[1] developed a cognitive machine-learning algorithm, trained with speckle tracking echocardiographic(STE) data, to differentiate constrictive pericarditis[2] from restrictive cardiomyopathy[2]. Narula[3] also showed that supervised learning algorithms could differentiate athlete heart and hypertrophic cardiomyopathy, using STE data, more accurately than traditional measure systems. Another potential field of application of ML models in echocardiography is heart valve disease(HVD). HVD is an increasingly common pathology that can benefit from cardiac imaging ML integration through early diagnosis, treatment, or surgery planning. B. Magnetic Resonance Imaging (MRI) In cardiac MRI, ventricular segmentation is one of the fields with more potential for the application of ML models. It makes it possible to quantify the volumetry and improve the efficiency and reproducibility of clinical assessments. Researcher Avendi[4] used deep learning algorithms trained through cardiac MRI datasets for the automatic detection and segmentation of the right ventricular chamber, foreseeing the accuracy of these algorithms. Likewise, for left ventricular segmentation, several automated neural networks(ANNs) have been successfully developed, especially for cardiac cine MRI. Another application of ML in cardiac MRI takes place in the detection of subacute or chronic myocardial scars. C. Cardiac Computed Tomography (CT scan) ML image analysis techniques in cardiac CT are increasingly used in the diagnosis and risk assessment of coronary artery disease and atherosclerosis. Coronary computed tomographic angiography is a noninvasive modality to detect coronary artery disease. To characterize coronary plaque, automatic coronary artery calcium scoring in CCTA using ML models provides added clinical value by reducing false-positive and interobserver variability. Researcher Gonzàles[5] used a convolutional neural network to calculate the Agatston score from CT without prior segmentation of coronary artery calcification. D. Electrocardiography An electrocardiogram (ECG) is commonly performed to test heart function in emergency room patients. The test can identify cardiac abnormalities but not failure. Automated ECG Interpretation Blood tests can be used to identify markers of cardiac failure but are unreliable. To help with diagnosis, Mayo Clinic researchers taught artificial intelligence to distinguish between ECG patterns of people ultimately diagnosed with heart dysfunction and those who were not. The AI-enhanced ECG performed better and faster at diagnosing dysfunction than standard blood tests. Risk Prediction Researchers used AI to identify a new biomarker for heart attack. Researchers first used fat biopsies from patients undergoing cardiac surgery to analyze genes associated with inflammation, scarring, and blood vessel formation. The expression of these genes was matched with coronary CT scan images to determine features indicating changes to the fat surrounding the heart. Researchers then used AI to develop the fat radiomic profile (FRP), which identifies red flags in the fat lining the blood supply to the heart. This new profile could be used to predict heart attacks in patients up to five years before they occur. AI-Aided Continuous Monitoring An AI wearable can help prevent up to a third of heart failure repeat hospital admissions. The device is worn by heart failure patients for up to three months after being discharged from the hospital and performs continuous ECGs. The AI establishes normal heart rate, heart rhythm, respiratory rate, and walking and sleep patterns for each patient. It then analyses deviations from these norms for indications the patient’s heart condition is worsening. The system was able to predict rehospitalization with 85% specificity up to 10 days before patients were readmitted. An AI hospital monitoring device has received approval for home use by patients with chronic obstructive pulmonary disease (COPD) and heart failure. The device monitors pulse, respiration, oxygen saturation, temperature, and mobility. The data is analyzed for warning signs, and healthcare providers are automatically alerted. A personal AI device is available for detecting atrial fibrillation (or AFib). The device is worn around the chest and performs continuous ECGs. AI interprets the data and alerts wearers to irregularities via mobile app. Individuals have control of their data and choose when to share it with their doctor. Research shows patients who wear monitoring devices are more likely to receive a timely diagnosis than those who receive standard care. Jeff Williams, Apple's chief operating officer, speaks about the Apple Watch Series 4 at the Steve Jobs Theater in Cupertino, California, U.S., on September 12, 2018. REUTERS/Stephen Lam/File Photo
AI is truly on the verge of redefining how cardiovascular care is delivered to patients. Companies and researchers have implemented AI in every step of the process, from continuous monitoring of basal heart rate for early warning signs to a quick and efficient noninvasive diagnosis of cardiac conditions. AI is also making later stages of the care pathway more efficient, such as real-time visualization of the cardiac anomaly and subsequent therapy selection. However, the question that remains to be answered is will this advanced technology, in the long run, bring down the cost and time of cardiovascular care for patients. Summary Artificial intelligence's arrival in the cardiovascular profession is bringing with it a variety of new opportunities for providing innovative, tailored care. The way we practice cardiology, particularly in the field of cardiac imaging, is changing, and physicians must be prepared. Tech companies are forging new links between patients and doctors, transforming healthcare from a passive to a pervasive activity. Physicians should not be terrified of AI's integration into cardiology; instead, they should embrace it because their specialist knowledge will always be important. Reference
Comments are closed.
|
Page HitsAuthorArchita Archives
January 2023
Categories |


 RSS Feed
RSS Feed